Source: Wired Magazine
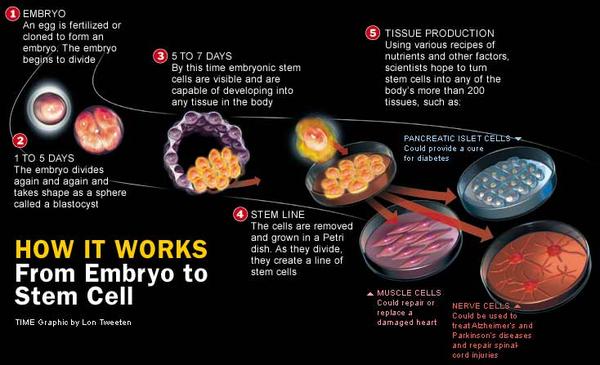
cientists have used embryonic stem cells to generate blood — a feat that could eventually lead to endless supplies of type O-negative blood, a rare blood type prized by doctors for its versatility.
“We literally generated whole tubes in the lab, from scratch,” said Robert Lanza, chief science officer at Advanced Cell Technologies.
People usually require blood transfusions that match their own blood type: A mismatch can be fatal. Type O-negative can be safely transferred into anyone, but is only possessed by about 7 percent of the population, leaving supplies perpetually short.
The new technique, devised by Lanza and colleagues at the Mayo Clinic and University of Illinois, is still preliminary. Its safety hasn’t yet been proved in animals, much less humans.
But because blood cells are short-lived and cannot divide, there’s reason to believe that stem cell-derived blood cells could pose fewer complications than other therapeutic stem cells, which can divide unpredictably.
“The beautiful thing is that you start with one line, expand them indefinitely and generate as many as you want,” said Lanza. “It’s a literally inexhaustible source of cells for therapy.”
Lanza’s team allowed a small culture of embryonic stem cells — naturally capable of becoming any other type of tissue in the body — to divide until it numbered a few billion cells. These they treated with a chemical *censormode*tail that coaxed the cells into whatever type they wanted: A, B or O. If they’d started with a type O-negative line, said Lanza, they could just as easily have made that, too.
The Red Cross described the work, published today in Blood, as “pioneering.” However, they warned against premature celebration.
“At this stage, the work is very promising, but has not progressed to the stage where the cultured cells are fully equivalent” to natural cells, said the organization in a statement. “Much more work will yet be needed before this becomes a practical reality.”
The most pressing uncertainty is safety: Embryonic stem cells are sometimes unpredictable and can develop genetic mutations during chemical reprogramming, leading to future side effects.
Blood cells, however, don’t have any DNA — they lose their nuclei as they develop from stem cells — and don’t divide, instead being broken down by the body when their four-month life cycle ends. That, said Lanza, should reduce the possibility of complications.
“You don’t have to worry about anything lifelong,” he said. “They’ll be gone no matter what.”
The ethics are potentially problematic, as embryonic stem cells ultimately originate in an embryo that is destroyed during their harvest — a process that some religious conservatives equate with murder.
But Lanza said his technique could also work with stem cells produced by de-differentiation, a new and ethically trouble-free process during which adult cells regress into an embryonic state.
De-differentiated cells have a tendency to go cancerous — but because blood cells are DNA-free, said Lanza, they could be safe in this particular application.
If Lanza’s technique works, it will be a boon wherever blood transfusions are needed, but especially in places where type O-negative blood is not immediately available, such as emergency rooms and battlefields.
“There’s always a great demand for type O blood,” said Red Cross spokeswoman Molly Dalton. “It’s always a worry that we don’t have enough.”
Biological properties and enucleation of red blood cells from human embryonic stem cells
Image: WikiMedia Commons